d0beb247-f59e-7634-78dc-f5f1bdaa570f flex-box container between col-100 0
fa267640-3df7-c062-fb5d-08943293a34f flex-box col-100 0
04e2f9f4-eeda-20d8-0f58-33ea5e88f2b2 col-100 0
Information
What is pulmonary fibrosis?
f503be75-8c77-7f77-11b4-415c9d28d198 flex-box container between col-100 0
3f73312a-cb6c-0b9c-19f5-9a92d6e7db4b flex-box col-50 0
5e8280aa-ae45-4512-c3ff-e8ed3aafaae1 col-100 0
Pulmonary fibrosis (PF) describes scar tissue in the lungs. This page explains what happens in the lungs, why some people get pulmonary fibrosis, symptoms of pulmonary fibrosis and treatments.
d2bafc88-277b-0ac4-d46c-18361f6e0b9b col-100 1
What is pulmonary fibrosis?
ffd0fc74-3333-4d87-4a73-5fbb81c63131 col-100 2
You might be told by your medical team you have ‘lung scarring’ or ‘pulmonary fibrosis’. On this page, we talk about pulmonary fibrosis.
The term pulmonary fibrosis describes scar tissue in the lungs.
Pulmonary – refers to the lungs
Fibrosis – refers to the scarring
Scar tissue can make it difficult for the lungs to work normally. Some people with interstitial lung disease (ILD) may develop pulmonary fibrosis.
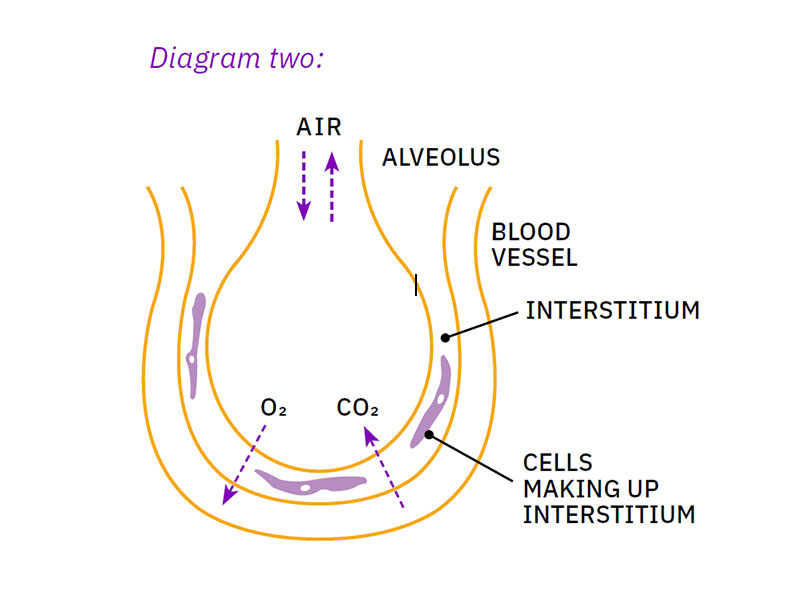
Interstitial lung disease: a group of diseases that affect the interstitium of the lungs. The interstitium is the space in the lungs between the air sacs (alveoli) and the blood vessels. (See diagrams 2 and 3).
b7d38135-ecc5-2339-20f4-7f029f4c6ae7 flex-box col-50 1
585f4317-0d5b-1b00-a660-c7610cbeb706 col-100 0
beef39fa-6597-f933-fec2-eecc831b60a6 flex-box container between col-100 0
f021a3d6-c048-705f-ebfb-dad234614c8a flex-box col-100 1
6ef72405-cb60-5541-b421-0b90f6530fe8 col-100 0
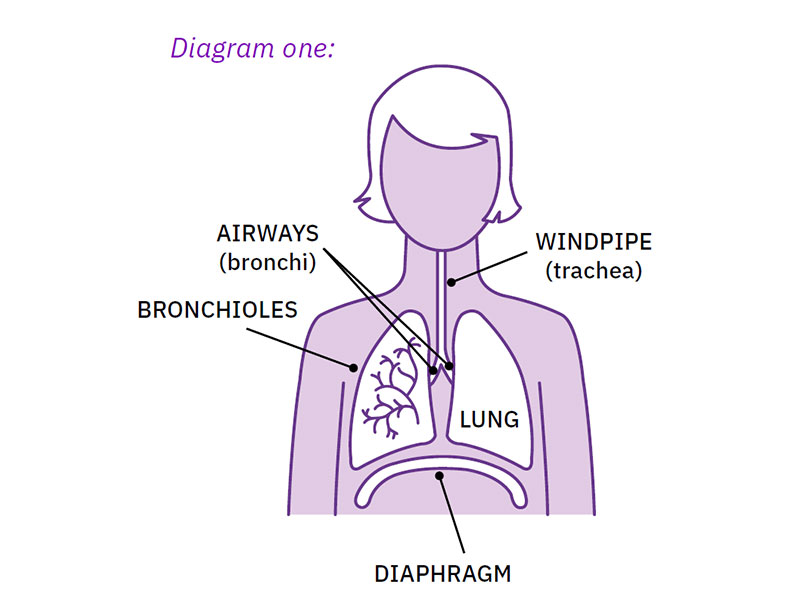
How do the lungs work?
Healthy lungs are spongy and stretchy so air can move in and out of them. There’s a network of tubes that carries air through the lungs. At the end of the tubes are small sacs called alveoli, surrounded by blood vessels. Oxygen and carbon dioxide move between the alveoli and the blood. The space between the alveoli and blood vessels is called the interstitium. This space contains different cells that help the lungs work properly.
faa1946f-6fb9-8d81-204f-5928c767132e flex-box col-50 2
50fc4c11-69d7-cb72-f1fc-af9ecef17042 col-100 0
f19f3ecb-bba6-53f7-6350-efc0aba885c7 flex-box col-100 3
9be8e880-984f-e72d-b159-d65d2dd5ffc7 col-100 0
e5ab868b-cfac-cfb5-d646-fbdb5fbf1d65 flex-box col-50 3
a2e9f1cd-0d1a-bf1b-8094-e011bf7406e7 col-100 0
33045e4e-a2a1-04c5-8233-49f14c8919fd flex-box container between col-100 0
05d05976-84d7-5f78-0f76-9fce0cd0fa42 flex-box col-100 0
e88078c7-8418-49f0-0a26-c8b7029d60ad col-100 0
What happens in the lungs when you have pulmonary fibrosis?
62ab3fd8-7983-2d83-bff1-bc6f0685e583 flex-box col-50 1
a59844a3-d3be-e911-b4c7-09054f2272b7 col-100 0
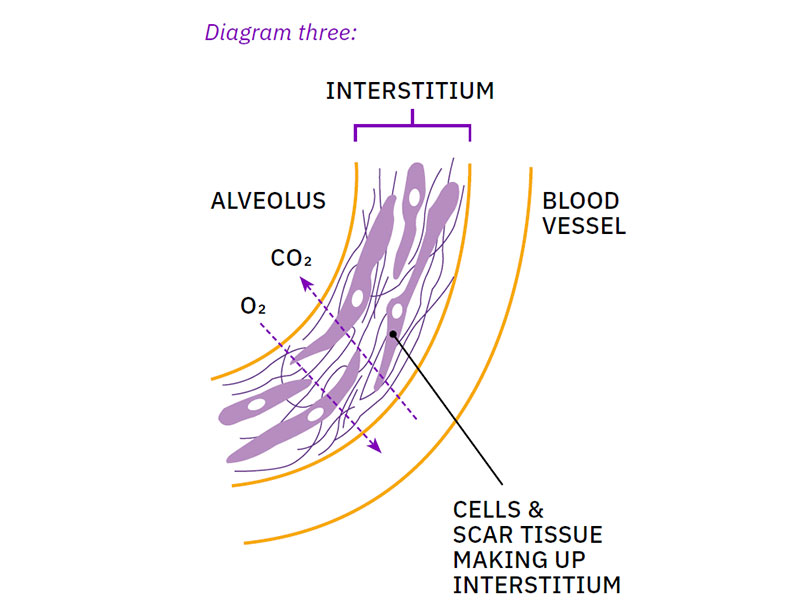
Scar tissue forms in the interstitium and this area becomes thicker. This makes the lungs stiff and less stretchy, which can make you feel short of breath (breathless). Several different mechanisms can cause a cough. Change to the structure of the lungs is one potential cause.
Scar tissue makes it more difficult for oxygen to move between the alveoli and the blood. Because of this, there is less oxygen available for the body to use.
97c7d270-770d-ef4f-25be-8ec0bb6e6519 flex-box col-50 2
8272b11a-5df5-bd9c-e10e-f6c02c1999af col-100 0
4ce1bffe-3de7-c432-b6bd-5e6ca4b43851 flex-box container between col-100 0
885e5fcf-2ce1-27f6-3199-fc3d0af80cc7 flex-box col-100 0
41806b05-0ff3-a4a4-99ee-98fc9460eb9c col-100 0
Why does lung scarring happen?
We don’t know exactly what happens in the lungs when someone has pulmonary fibrosis. There’s more research looking into this. From what we have learned so far, two processes can lead to scar tissue in the lungs:
cd4aa848-4606-9d3c-c9a3-9b8dd058bd98 col-100 1
Inflammation
Inflammation is when something causes irritation or injury to the lungs. Some types of ILDs can cause inflammation in the lungs. These ILDs include, but are not limited to, sarcoidosis autoimmune disease-associated ILDs, and hypersensitivity pneumonitis. Inflammation can lead to scar tissue in the lungs (pulmonary fibrosis).
d1a429b4-8b6b-c396-c151-55c7cdb0f84e col-100 2
Lung cells age too quickly
Pulmonary fibrosis can happen when cells in the lungs age too quickly.
One of the normal functions of these cells is to repair damage. Ageing lung cells are unable to repair normally. Instead, they cause scar tissue to form. So, factors that cause lung cells to age too quickly increase the risk of pulmonary fibrosis. This includes genes (inherited from your parents), your environment (e.g. dust or smoke that your lungs have breathed in previously), and other risk factors below. Read about risk factors in the next section.
Damage to lung cells is normal. We breathe in over 10,000 litres of air each day. Air may contain dust, pollutants, viruses, bacteria or small amounts of stomach content. These can damage the delicate lining of the lungs. Cells that are lost to damage must be replaced. When a person has pulmonary fibrosis, their body is not able to replace cells as it normally would.
People around the world are working to improve the lives of those affected by pulmonary fibrosis. Sign up for our e-newsletter to learn about the amazing work happening to improve pulmonary fibrosis care, discover more about the disease and help people live well.
06860713-6ffc-0f1e-d04d-dfe72c93ffd0 flex-box container between col-100 0
b0540110-1ad1-3733-83e1-21aea8d261d7 flex-box col-100 0
82864efb-0dde-de22-ec41-593f67f685e3 col-100 0
People around the world are working to improve the lives of those affected by pulmonary fibrosis. Sign up for our e-newsletter to learn about the amazing work happening to improve pulmonary fibrosis care, discover more about the disease and help people live well.
3955ce84-d563-829f-e92c-9b9d46ad8e87 flex-box container between col-100 0
ecc35e1c-7ac7-f5d4-557f-d149b6c86fd5 flex-box col-100 0
7115625f-bbc6-c20f-b186-265b1d5eaf12 col-100 0
What causes pulmonary fibrosis?
From what we have learned so far, there is no single cause of pulmonary fibrosis. Instead, we talk about different risk factors. Risk factors can lead to inflammation or lung cells ageing too quickly. This can increase the risk of scarring.
b1f04bca-b464-9a6d-15dc-1971a6fbb11c flex-box col-100 1
14298537-1502-e973-8cdb-1d745ec78b35 col-100 0
Pulmonary fibrosis risk factors
c174e0c0-b71c-5b78-14b8-a62d1b6c56fa flex-box col-50 2
87157c9d-a439-9c98-f393-fa03022881d3 col-100 1
Risk factors for pulmonary fibrosis can include:
3e28fe9d-1b16-b842-630c-d79105645b39 col-100 2
Many people with pulmonary fibrosis have a combination of risk factors. Your medical team will try to find your risk factors. This helps them diagnose the correct type of pulmonary fibrosis.
8e8bd582-2f76-ed2f-2b22-9c619651480d flex-box col-50 3
2c6f5332-9f38-d982-b93f-2cde34fd57b8 col-100 0
b3f5ac49-6246-8aba-12ff-82a87385ae94 flex-box container between col-100 0
99018eaa-4dfd-77b2-1690-a540084b6a03 flex-box col-100 0
2946185e-4b77-7b5a-f336-087c86a53726 col-100 0
Diseases involving pulmonary fibrosis
6e68dc68-b5ae-7d99-69e7-602a9b16a19c flex-box col-50 1
348439f8-a21c-d9f6-89d4-c42cbfab497f col-100 0
There are several different diseases that involve pulmonary fibrosis. These are called interstitial lung diseases (ILDs). Your medical team will use information from scans, tests and your medical history to decide which ILD you have. You can read more about this in the Diagnosis section below.
fd1a425c-931f-8b68-6a53-1573cb045396 col-100 1
Your medical team may check if your pulmonary fibrosis changes. This is to see if your disease is progressing. It’s important to know this to help determine the right support and treatment for you.
Not everyone with pulmonary fibrosis will get worse.
83a9a440-324b-c114-8e74-a3bcdf9ab43d flex-box col-50 2
533547b2-62bf-e4da-465d-1540bac39d6a col-100 0
Progressive pulmonary fibrosis
Progressive pulmonary fibrosis gets worse with time.
46527b99-de98-6573-9368-1520e2479205 col-100 1
Non-progressive pulmonary fibrosis
Non-progressive pulmonary fibrosis is the result of a one-off event. It does not get worse over time.
c20ba15d-b302-cfae-2a8a-12b5bd938d5a flex-box container between col-100 0
01dca8ff-d675-f41f-471e-40041d7758a0 flex-box col-100 0
21eaa024-ffd6-b018-73ea-84b81b635738 col-100 0
Diagnosing pulmonary fibrosis
35426aef-e822-ff3b-5035-5dad7f2dfaff flex-box col-50 1
58776074-54d3-a727-95da-a1794f6c8604 col-100 0
Who is involved in the diagnosis?
A doctor will diagnose pulmonary fibrosis. They are often part of a specialist ILD multi-disciplinary team (MDT).
And MDT is a team of different healthcare professionals.
2afbfc95-a3c5-d6b1-d11a-8a6a1297318a col-100 1
Tests and scans to gather information
The healthcare professionals involved in your diagnosis will gather information in different ways. This may include:
96250fdc-c599-5694-68a7-20e83cf5ffe6 col-100 2
- asking questions about your symptoms, and your personal and family medical history
- asking questions about situations where you might have breathed in something that can irritate the lungs
- a physical examination. This could include listening to your breathing with a stethoscope
- further tests, which may include pulmonary (lung) function tests or a computerised tomography (CT) scan
cbbc9c80-e40c-e739-dcfb-497a25008f06 flex-box col-50 2
3f5039ef-14a5-e77a-b47c-586d09544139 col-100 0
f9b4733e-9b2d-bfff-b042-1848415e9fc3 col-100 1
CT scan: Combines lots of X-rays to create a more detailed image.
Sometimes, you might need other procedures to help determine the type of lung disease. These procedures might include a bronchoscopy (a camera into the lungs) or lung biopsy (taking a sample of lung tissue). The team will discuss this with you.
The information your medical team find will help them make the most likely diagnosis.
ee2aa684-45df-87e1-2511-3ab850221a79 flex-box container between col-100 0
57e98da6-2eeb-e0c6-0353-1cdda04619b5 flex-box col-100 0
74d1f785-2395-332b-2b6c-4d00342a0c64 col-100 0
What are pulmonary fibrosis signs and symptoms?
71efe22e-078b-46a5-c304-a31c04e47535 col-100 1
You might be told by your medical team you have ‘lung scarring’ or ‘pulmonary fibrosis’. On this page, we talk about pulmonary fibrosis.
d0fed58d-e61a-0e59-4ff1-c04de7c23514 col-100 2
The signs and symptoms of pulmonary fibrosis vary from person to person. They may also change if the disease progresses.
9e19bb1c-6635-1876-0407-13939e4d91c3 flex-box col-100 1
5b30b7b7-0a8d-c633-e99f-409fe243afb9 col-100 0
Pulmonary fibrosis signs
Signs: information that healthcare professionals find.
A common sign is hearing crackles when listening to your breathing with a stethoscope. This sounds similar to Velcro being pulled apart.
370146d3-bf83-5f95-b988-550af4fe3837 flex-box col-50 2
747a6744-b915-91d0-46b0-9fe5fe368f0c col-100 0
Pulmonary fibrosis symptoms
Symptoms: your experience of pulmonary fibrosis.
Common symptoms can include:
0514ca11-5120-2077-c9c5-53836d28c960 col-100 1
- shortness of breath (breathlessness)
- dry cough
- tiredness (fatigue)
- unexplained weight loss
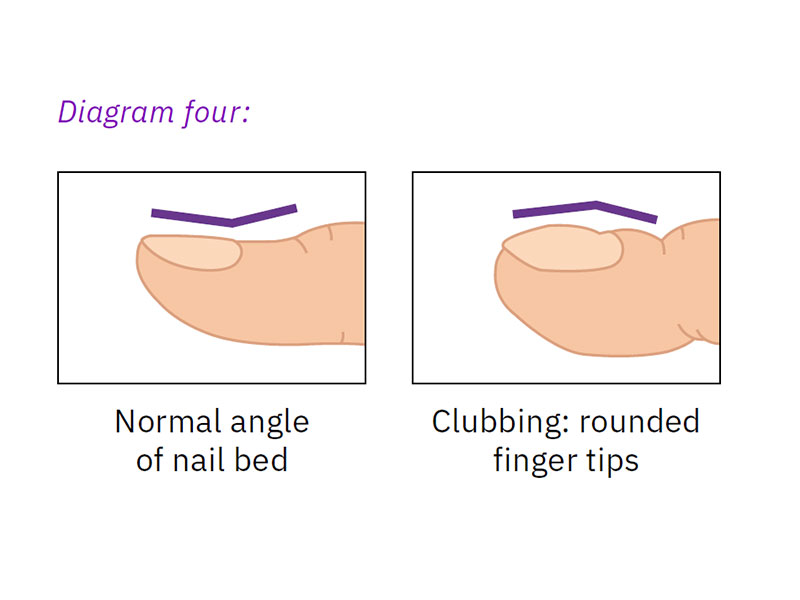
- clubbing of fingers and toes (swollen and rounded finger and toe tips – see diagram four)
01e7913d-819c-9cbb-980c-5106b31d3bb4 flex-box col-50 3
8c03b8f8-b560-48ed-a7db-cec1edd741a2 col-100 0
218f95f3-96ea-3e78-e8e9-f7c90b719791 flex-box container between col-100 0
09c5a524-9539-6621-d7fc-91a0f659fc75 flex-box col-100 0
39764421-46d1-2e34-67f0-fca3bfa69bb2 col-100 0
Are there treatments for pulmonary fibrosis?
d8fc4b6a-dcaf-5c89-339f-92bcd7b0e89f flex-box col-50 1
17d108f8-471b-5144-20c8-23ad6d5e1ffe col-100 0
Currently, we can’t stop pulmonary fibrosis. However, some treatments can slow down the rate of further scarring. Other treatments can help to manage your symptoms. Not all treatments are suitable for everyone, so your medical team will discuss the best treatments for you. Some people have pulmonary fibrosis that is not progressive and might not need treatment.
fd068fd1-74a7-aae6-7583-db9e27ceb0a5 col-100 1
Possible treatments may include:
e95f9022-0747-28f9-841f-0876e0929c7d flex-box col-50 2
00345930-a090-cdf5-50fe-7a8e134537ef col-100 0
eea636c7-235c-5415-2174-51e43efa7ba0 flex-box container between col-100 0
0ae07434-ea6e-d809-7e79-a2add5882839 flex-box col-50 0
e5a7f606-dd77-71f5-7a1a-948c3edfe041 col-100 0
Possible symptom management
332f51d0-2938-9702-6c91-e5a15f328664 col-100 1
ee24bc5a-0732-e3e9-4bf1-babaa35fffd8 flex-box col-50 1
7eba02e4-bebc-bbac-d647-35e1b74f8dad col-100 0
Living well with pulmonary fibrosis
22b0d41b-a349-4ab3-b278-563148c1c791 col-100 1
Everyday choices can help you live well with pulmonary fibrosis.
This might include:
ab563378-a97c-d950-600f-9880b41650df col-100 2
373659aa-730a-9649-8700-b1d5d4c48469 flex-box col-100 mrg-t-reg 2
025912c9-92c3-4da6-5bf8-345355ffe4d3 col-100 0
Learn more about living well with pulmonary fibrosis by signing up for Insider magazine. Read stories about how people manage pulmonary fibrosis alongside their work, hobbies or family, and information from experts on living well.
f28117ee-ef58-472b-af42-ca65a8ed53f4 flex-box container between col-100 0
17ceb33f-1d2e-ad72-b27c-89bb5aa86f3c flex-box col-100 0
a58a2e74-e6e9-7875-c160-769c1b688e5c col-100 0
3e6c4fad-7faf-fe70-71af-38d48131fe3b flex-box col-100 mrg-b-lrg 1
d21bbb62-72e4-aa65-4f84-415d9a58793c col-100 0
Why is pulmonary fibrosis research important?
4fc1b5c5-0cc7-7d6e-579d-c3279a9e93ef col-100 1
Research studies and clinical trials help us to:
- learn about pulmonary fibrosis
- find new treatments
- improve clinical services and care
97aaf923-ba68-f6d8-29b3-22e8bb32c64a flex-box col-100 2
f419cad4-0afc-ff80-0fe1-0b29b54c072d col-100 0
How to get involved in pulmonary fibrosis research
1bd4b6dc-cd40-eb5b-81b6-8366ba7d457e col-100 1
People living with pulmonary fibrosis tell us that being involved in research can be a rewarding experience. By getting involved, you can:
18895666-32db-e037-6d80-daecd1e9a472 col-100 2
- gain a better understanding of pulmonary fibrosis
- build links with medical teams
- access new treatments
- help others with the disease
a51eb934-4a41-c26c-0b1a-fde46efbf274 col-100 3
Learn about the exciting research happening in the UK today, and see what you can get involved in.
8a7847ce-6f56-3554-4015-983571beffc7 mrg-b-lrg 4
Find a research study now65e1ca8f-4b5a-7d65-63ef-c0c6e01d4e1d col-100 5
Or speak to your ILD team about opportunities to get involved in research.
8e778d22-fc19-f43a-744d-8095d263c753 flex-box container between col-100 0
05066d16-83f5-2d60-cae7-ba1d070b5f0f flex-box col-100 0
10e59480-6a34-582c-9092-7a6073e28a9b col-100 0
Pulmonary fibrosis life expectancy
874ba81f-c24f-37c9-f564-419a71b33295 flex-box col-50 1
b1d7e1f3-0011-96ff-202b-ad61e89e316b col-100 0
Learning about life expectancy
782a8d97-532e-26b3-0ca7-c23616f60a6a col-100 1
Reading about life expectancy can be difficult. You might want to read this information with someone you trust and who can support you. The APF support line is also here for you.
78c027ce-54d4-1c6c-09bd-3b854c76409b 2
Contact our friendly Support line teamd44e529d-f49b-5f1a-272b-34554f731932 flex-box col-50 2
6cb53bd5-7b06-293e-f5e3-37f4006b0f78 col-100 0
What are the stages of pulmonary fibrosis?
a5d49115-c664-b060-6499-b7bc17b27c0a col-100 1
Pulmonary fibrosis can be a progressive condition, meaning it can get worse over time. Not everyone has progressive pulmonary fibrosis. Progression can look different for everyone. Your symptoms may stay the same for a long time or get worse quickly.
160d3164-1260-1b8f-fe8c-a746e10290bc flex-box container between col-100 0
23da28b6-be21-4145-2f2b-12134b7e74f2 flex-box col-100 between 0
34218bf2-8c78-19b2-6831-be9713225e30 col-100 0
How long will I live with pulmonary fibrosis?
c6149e2b-b3df-6b36-7915-a9cb5d630623 col-100 1
Pulmonary fibrosis that gets worse is a terminal disease (sometimes also called ‘life-limiting’). This means there is currently no cure. Many people who are diagnosed with the disease will eventually die from it.
45a29a58-b4bf-502f-f610-2e0418dfd58e col-100 mrg-b-lrg 2
Many factors affect how long a person may live with pulmonary fibrosis, including:
- how severe your lung scarring is when you are diagnosed
- how quickly your pulmonary fibrosis gets worse (if your disease gets worse)
- your other health conditions
- if you get infections
- your lifestyle, e.g. if you smoke
a479cb44-4e14-049f-151a-be5b7f53155d col-100 3
It’s important to note that life expectancy research needs updating. It may no longer be accurate. Previous research looked at the average life expectancy of people with idiopathic pulmonary fibrosis (IPF). Life expectancy was suggested to be 3-5 years from diagnosis. However, researchers found this number before antifibrotic medications were widely used. At this time, diagnosis also took longer, and less was known about the disease.
There is also little information on the life expectancy of people with other types of pulmonary fibrosis.
There have been huge improvements in pulmonary fibrosis treatment and care. However, it’s important to acknowledge there is still work to do. This will ensure timely access to care and better treatments. Researchers are working to understand why pulmonary fibrosis happens and to find more effective treatments.
a8babe02-fd63-6846-a2de-bc27d8bbb701 flex-box container between col-100 0
c0b6eada-4cc3-ae9c-184e-b013ca7039f3 flex-box col-100 0
90876a00-5db5-68ab-ff01-77f7fcd173b6 col-100 0
Pulmonary fibrosis support
b7300189-653a-f4c3-b8c9-b537036e1126 col-100 1
It’s understandable to have questions or concerns about your life expectancy. Your medical team are there to support you and answer questions about your personal situation. They can also help you manage your symptoms and live a healthy lifestyle. This can improve your health and chances of living well with pulmonary fibrosis. Read more about living well in the Treatment section.
f8d14146-e7fd-4b04-b349-f1acf061d1c2 flex-box col-50 1
102c0822-df1e-eb5a-0eea-cd825f24d803 col-100 0
Join a support group
0155906d-5888-5afe-4f92-1b35f7faf976 col-100 1
It’s important to remember that you are not alone. There are now over 89 pulmonary fibrosis support groups around the country. Support groups meet informally to share experiences, provide expert information and raise funds and awareness.
5cd9c1ca-6aa9-f157-9688-c9b5d5febba7 mrg-b-lrg 2
Find a support groupd9072cd6-6029-2014-bef1-90c50e221bbe flex-box col-50 2
b20fd617-fd7f-71b1-ef02-f0e4c5973c19 col-100 0
Call our support line
13183024-2355-4e01-2c5c-93357efa0fb6 col-100 1
Our friendly Support line team are here for people living with pulmonary fibrosis, carers, family members and health and social care professionals. They can provide information on living with pulmonary fibrosis, emotional and practical support, and signposting to helpful services and organisations.
aaee937d-3e6b-f1f9-efdf-593f5b867c5d mrg-b-lrg 2
Call or email the Support line0ee2ab8e-4a40-e092-2687-4c7191fe2d9c flex-box col-50 3
13602c59-07b7-1dce-e21a-b036109c3e99 col-100 0
Find us on social media
42f1a0f8-93e4-b97d-16b6-030db82f9b93 col-100 1
We have an active and supportive online community ready to welcome you on Facebook, Twitter and Instagram for updates, news and connections to our online community.
9591347b-3302-7e76-8864-0454da59bbb2 flex-box col-50 4
31b1d019-3ced-8de7-304f-e17143f9cd72 col-100 0
Join our webinars on pulmonary fibrosis
8ee60f1f-5358-96a8-4dab-4f50d5920924 col-100 1
Our pulmonary fibrosis webinars include in depth talks, patient stories, and insight from healthcare professionals.
51afe2e4-7230-9e36-ab3d-6e815400d387 flex-box col-100 5
9c3ff8e0-b2e7-db73-9344-88d9ee258532 col-100 0

The work APF is doing for individuals and families affected by PF is great and I would like to help in any way I can.

3a93a3fe-4472-32af-9d8c-6f7a57410324 flex-box container between col-100 0
444567ee-f547-0012-ab00-87b3c9bc2c95 flex-box col-100 0
83ba2ead-4bc7-7502-0d3f-5306c4eb3afb col-100 0
For healthcare professionals
7b4801dc-dcdb-6c49-3e7a-60b9cdc6f925 col-100 1
Find resources for your patients, opportunities to influence care pathways and much more on our Healthcare Professional Hub.
7f7cc5ac-ce2e-c607-fec2-f8e244f01872 mrg-b-lrg 2
Information and resources for HCPs027bdf7a-071e-cf7d-a68f-288f918ad0e1 col-100 3
Our website and resources provide general information only. We cannot provide medical advice, treatment or prescriptions, nor can we assess/decide what services or clinicians you should be referred to. Support with these matters will need to be provided by your existing healthcare professional teams.
APF is not responsible for any errors or omissions or for any loss or damage suffered by users resulting from the information published on our website or in our resources.
Tab ID:174